Specific Health Concern >> Heartburn
 To Request an Action Plan to address Low Back Pain Click Here
To Request an Action Plan to address Low Back Pain Click Here
To attend a FREE Class on this topic, Click Here
In this video, Dr. Huntoon discusses the 4 Causes of All Health Concerns and helps you to understand that having any symptoms are not normal.
Click on the link below to listen to the radio show about the Stomach.
When you are ready to address the cause of your Heartburn, we are here to serve you.
![]() To Request an Action Plan to
To Request an Action Plan to
Address Heartburn Click Here
Heartburn / Gastroesophageal Reflux Disease
Gastroesophageal Reflux Disease (GERD) is a more serious form of Gastroesophageal Reflux (GER), which is common. GER occurs when the lower esophageal sphincter (LES) opens spontaneously, for varying periods of time, or does not close properly and stomach contents rise up into the esophagus.
GER is also called acid reflux or acid regurgitation, because digestive juices—called acids—rise up with the food. The esophagus is the tube that carries food from the mouth to the stomach. The LES is a ring of muscle at the bottom of the esophagus that acts like a valve between the esophagus and stomach.
When acid reflux occurs, food or fluid can be tasted in the back of the mouth. When refluxed stomach acid touches the lining of the esophagus it may cause a burning sensation in the chest or throat called heartburn or acid indigestion.
Occasional GER is common and does not necessarily mean one has GERD.
Persistent reflux that occurs more than twice a week is considered GERD, and it can eventually lead to more serious health problems. People of all ages are susceptible to the condition.
Symptoms
The main symptom of GERD in adults is frequent heartburn, also called acid indigestion—burning-type pain in the lower part of the mid-chest, behind the breast bone, and in the mid-abdomen.
Most children under 12 years with GERD, and some adults, have GERD without heartburn. Instead, they may experience a dry cough, asthma symptoms, or trouble swallowing.
Causes
The reason some people develop GERD is still unclear. However, research shows that in people with GERD, the LES relaxes while the rest of the esophagus is working. Anatomical abnormalities such as a hiatal hernia may also contribute to GERD. A hiatal hernia occurs when the upper part of the stomach and the LES move above the diaphragm, the muscle wall that separates the stomach from the chest. Normally, the diaphragm helps the LES keep acid from rising up into the esophagus. When a hiatal hernia is present, acid reflux can occur more easily. A hiatal hernia can occur in people of any age and is most often a common finding in otherwise healthy people over age 50. Most of the time, a hiatal hernia produces no symptoms. 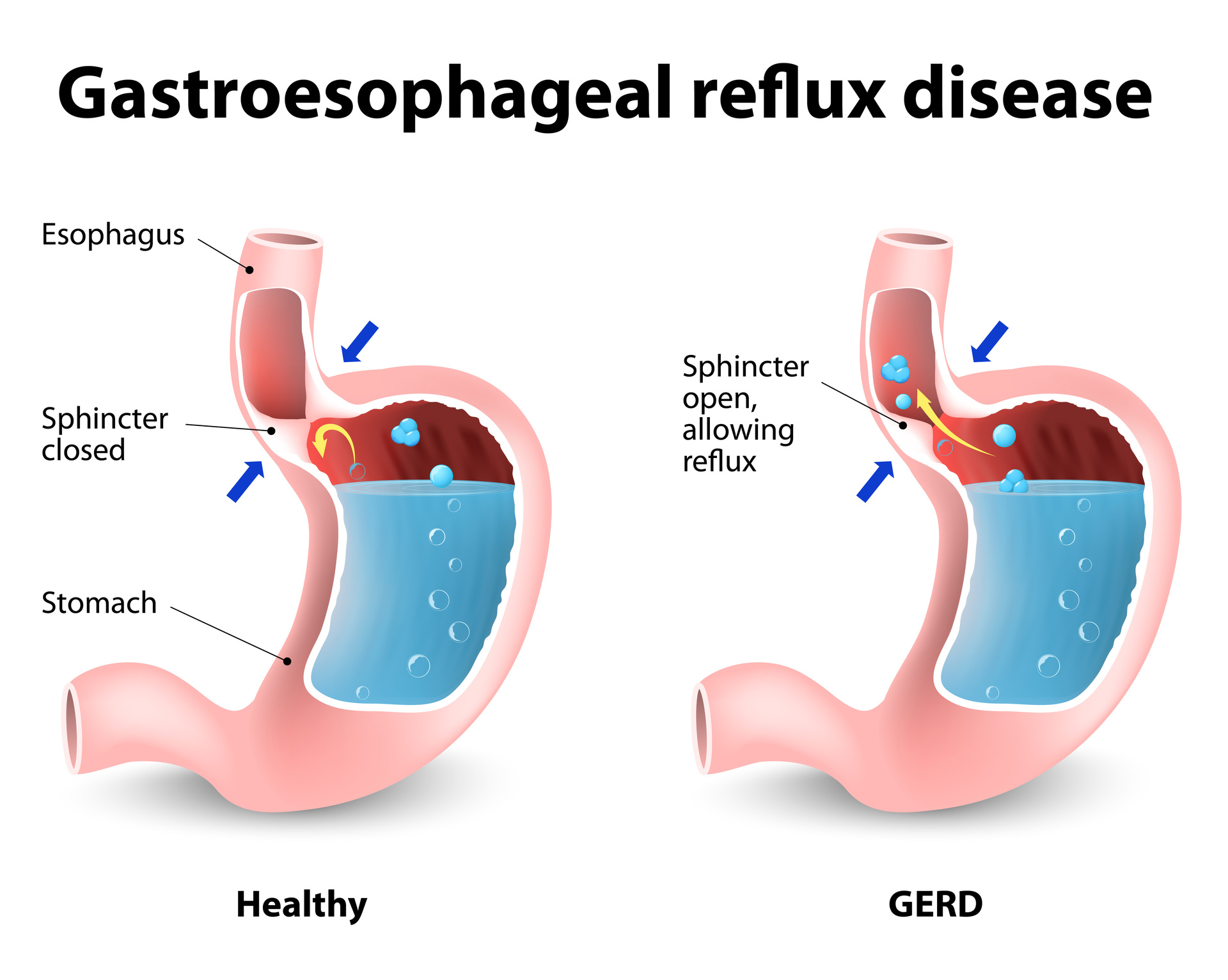 Other Factors that may Contribute to GERD include:
Other Factors that may Contribute to GERD include:
- food allergies
- gall bladder dysfunction
- obesity
- pregnancy
- Smoking
Common Foods that can Worsen Reflux Symptoms include:
- any food allergy
- citrus fruits
- chocolate
- drinks with caffeine or alcohol
- fatty and fried foods
- garlic and onions
- mint flavorings
- spicy foods
- tomato-based foods, like spaghetti sauce, salsa, chili, and pizza
What is GERD in Children?
Distinguishing between normal, physiologic reflux and GERD in children is important. Most infants with GER are happy and healthy even if they frequently spit up or vomit. This is usually due to food sensitivities or allergies to mother’s breast milk or formula. Babies usually outgrow GER by their first birthday. Reflux that continues past 1 year of age may be GERD. Studies show GERD is common and may be overlooked in infants and children. For example, GERD can present as repeated regurgitation, nausea, heartburn, coughing, laryngitis, or respiratory problems like wheezing, asthma, or pneumonia. These are classic allergy symptoms associated with what they are eating. Infants and young children may demonstrate irritability or arching of the back, often during or immediately after feedings. Infants with GERD may refuse to feed and experience poor growth.
Talk with your child’s healthcare provider if reflux-related symptoms occur regularly and cause your child discomfort. Checking your child for food allergies or sensitivities with a Holistic Chiropractor is the best place to start. Your healthcare provider may recommend simple strategies for avoiding reflux, such as burping the infant several times during feeding or keeping the infant in an upright position for 30 minutes after feeding. If your child is older, your healthcare provider may recommend that your child eat small, frequent meals and avoid the following foods:
- sodas that contain caffeine
- chocolate
- peppermint
- spicy foods
- acidic foods like oranges, tomatoes, and pizza
- fried and fatty foods
Avoiding food 3 to 4 hours before bed may also help. Your healthcare provider may recommend raising the head of your child's bed with wood blocks secured under the bedposts. Just using extra pillows will not help. If these changes do not work, your medical doctor may prescribe medicine for your child. In rare cases, a child may need surgery. For information about GER in infants, children, and adolescents, see the Gastroesophageal Reflux in Infants and Gastroesophageal Reflux in Children and Adolescents fact sheets from the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK).
Traditional Medical Treatment Options and Diagnosis
How is GERD Treated?
See your healthcare provider if you have had symptoms of GERD and have been using antacids or other over-the-counter reflux medications for more than 2 weeks. Your healthcare provider may refer you to a gastroenterologist, a doctor who treats diseases of the stomach and intestines. Depending on the severity of your GERD, treatment may involve one or more of the following.
Medications
Your medical health care provider may recommend over-the-counter antacids or medications that stop acid production or help the muscles that empty your stomach. You can buy many of these medications without a prescription. However, see your healthcare provider before starting or adding a medication.
- Antacids, such as Alka-Seltzer, Maalox, Mylanta, Rolaids, and Riopan, are usually the first drugs recommended to relieve heartburn and other mild GERD symptoms. Many brands on the market use different combinations of three basic salts— magnesium, calcium, and aluminum—with hydroxide or bicarbonate ions to neutralize the acid in your stomach. Antacids, however, can have side effects. Magnesium salt can lead to diarrhea, and aluminum salt may cause constipation. Aluminum and magnesium salts are often combined in a single product to balance these effects.
- Calcium carbonate antacids, such as Tums, Titralac, and Alka-2, can also be a supplemental source of calcium. Unfortunately, the calcium will not be absorbed or utilized by the body, since the antacid effect blocks the absorption of calcium. They can cause constipation as well.
- Foaming agents, such as Gaviscon, work by covering your stomach contents with foam to prevent reflux. This too will prevent proper absorption of nutrients and lead to other complications with your health.
- H2 blockers, such as cimetidine (Tagamet HB), famotidine (Pepcid AC), nizatidine (Axid AR), and ranitidine (Zantac 75), decrease acid production. They are available in prescription strength and over-the counter strength. These drugs provide short-term relief and are effective for about half of those who have GERD symptoms. They also cause decreased calcium absorption which may lead to osteoporosis and immune system weakness.
- Proton pump inhibitors include omeprazole (Prilosec, Zegerid), lansoprazole (Prevacid), pantoprazole (Protonix), rabeprazole (Aciphex), and esomeprazole (Nexium), which are available by prescription. Prilosec is also available in over-the-counter strength. Proton pump inhibitors are more effective than H2 blockers and can relieve symptoms and heal the esophageal lining in almost everyone who has GERD. There are side-effects to using these which should be considered fully before going on these medications.
- Prokinetics help strengthen the LES and make the stomach empty faster. This group includes bethanechol (Urecholine) and metoclopramide (Reglan). Metoclopramide also improves muscle action in the digestive tract. Prokinetics have frequent side effects that limit their usefulness — fatigue, sleepiness, depression, anxiety, and problems with physical movement.
Because drugs work in different ways, combinations of medications may help control symptoms. People who get heartburn after eating may take both antacids and H2 blockers. The antacids work first to neutralize the acid in the stomach, and then the H2 blockers act on acid production. By the time the antacid stops working, the H2 blocker will have stopped acid production. Your medical health care provider is the best source of information about how to use medications for GERD. Many Pharmacists are a wealth of information too, especially when taking multiple medications. Most important to consider is when stopping acid production in your stomach, this stops your ability to absorb calcium which will lead to many other conditions such as osteoporosis and weakened immunity. Consider this before taking any medication for GERD.
As with all medication, certain side-effects are known and others are not known. It is important to consider the side-effects and to do some research into the medication being prescribed to determine if the side-effects are worse than the symptoms associated with your GERD. Talking with your medical doctor or pharmacist is warranted. Considering Alternative treatments before starting stronger medication is best.
Medicines Two Choices for You
Dr. Huntoon's Alternative Medical Treatment Options
Dr. Huntoon has quite extensive experience in addressing this condition by locating the underlying cause. In just about every case over 27 years of this condition, the person has a dysfunctional gallbladder secondary to having a parasite. When addressing this aspect of a person's health, along with resetting the gallbladder circuit, this condition always resolves once and for all.
Lifestyle Changes
- If you smoke, stop.
- Avoid foods and beverages that worsen symptoms.
- Lose weight if needed.
- Eat small, frequent meals.
- Wear loose-fitting clothes.
- Avoid lying down for 3 hours after a meal.
- Raise the head of your bed 6 to 8 inches by securing wood blocks under the bedposts. Just using extra pillows will not help.
By working with a Holistic Chiropractor who can help you address the underlying cause of your GERD and removing the basis for the symptoms (hiatal hernia) will go a long way to fully resolving your GERD and its associated symptoms. Addressing the reasons for your digestive system imbalances is warranted.
What to Discuss with Your Doctor
Signs and Tests
See your healthcare provider if you have had symptoms of GERD and have been using antacids or other over-the-counter reflux medications for more than 2 weeks. Your healthcare provider may refer you to a gastroenterologist, a doctor who treats diseases of the stomach and intestines.
What if GERD Symptoms Persist?
If your symptoms do not improve with lifestyle changes or medications, you may need additional tests.
Barium swallow radiograph uses x rays to help spot abnormalities such as a hiatal hernia and other structural or anatomical problems of the esophagus. With this test, you drink a solution and then x rays are taken. The test will not detect mild irritation, although strictures—narrowing of the esophagus—and ulcers can be observed.
Upper endoscopy is more accurate than a barium swallow radiograph and may be performed in a hospital or a doctor’s office. The doctor may spray your throat to numb it and then, after lightly sedating you, will slide a thin, flexible plastic tube with a light and lens on the end called an endoscope down your throat. Acting as a tiny camera, the endoscope allows the doctor to see the surface of the esophagus and search for abnormalities. If you have had moderate to severe symptoms and this procedure reveals injury to the esophagus, usually no other tests are needed to confirm GERD.
The Doctor also may Perform a Biopsy.
Tiny tweezers, called forceps, are passed through the endoscope and allow the doctor to remove small pieces of tissue from your esophagus. The tissue is then viewed with a microscope to look for damage caused by acid reflux and to rule out other problems if infection or abnormal growths are not found. pH monitoring examination involves the doctor either inserting a small tube into the esophagus or clipping a tiny device to the esophagus that will stay there for 24 to 48 hours. While you go about your normal activities, the device measures when and how much acid comes up into your esophagus. This test can be useful if combined with a carefully completed diary— recording when, what, and amounts the person eats—which allows the doctor to see correlations between symptoms and reflux episodes. The procedure is sometimes helpful in detecting whether respiratory symptoms, including wheezing and coughing, are triggered by reflux.
A completely accurate diagnostic test for GERD does not exist, and tests have not consistently shown that acid exposure to the lower esophagus directly correlates with damage to the lining.
Surgery
Surgery is an option when medicine and lifestyle changes do not help to manage GERD symptoms. Surgery may also be a reasonable alternative to a lifetime of drugs and discomfort.
Medicines Two Choices for You
Prevention and Quick Tips
Frequent heartburn, also called acid indigestion, is the most common symptom of GERD in adults. Anyone experiencing heartburn twice a week or more may have GERD, and ultimately will have a parasite affecting their gallbladder.
You can have GERD without having heartburn. Your symptoms could include a dry cough, asthma symptoms, or trouble swallowing. This is tell-tale for a Hiatal Hernia.
If you have been using antacids for more than 2 weeks, it is time to see your healthcare provider. Developing a healthy life-style with proper guidance from your Holistic Chiropractor is the best prevention when considering how to approach your health.
Most doctors can treat GERD. Your healthcare provider may refer you to a Gastroenterologist, a doctor who treats diseases of the stomach and intestines.
Health care providers usually recommend lifestyle and dietary changes to relieve symptoms of GERD. Many people with GERD also need medication. Surgery may be considered as a treatment option.
Most infants with GER are healthy even though they may frequently spit up or vomit. This is most likely due to food allergies related to breast milk or formula. Most infants outgrow GER by their first birthday. Reflux that continues past 1 year of age may be GERD.
The persistence of GER along with other symptoms—arching and irritability in infants, or abdominal and chest pain in older children—is GERD. GERD is the outcome of frequent and persistent GER in infants and children and may cause repeated vomiting, coughing, and respiratory problems.
Hope through Research
Dr. Huntoon has quite extensive experience in addressing this condition by locating the underlying cause. In just about every case over 27 years of this condition, the person has a dysfunctional gallbladder secondary to having a parasite. When addressing this aspect of a person's health, along with resetting the gallbladder circuit, this condition always resolves once and for all.
The Medical reasons certain people develop GERD and others do not remain unknown. Several factors may be involved, and research is under way to explore risk factors for developing GERD and the role of GERD in other conditions such as asthma and laryngitis.
Participants in clinical trials can play a more active role in their own health care, gain access to new research treatments before they are widely available, and help others by contributing to medical research. For information about current studies, visit www.ClinicalTrials.gov.
More About AAMC
About Dr. Huntoon
When Your Health Matters
Click the link for a description of this week's show and a link to the podcast from:
Free Health Care Class Schedule
Classes start at 6: 30 pm
Classes are open to the public
You Must Call 845-561-2225
for reservations
Advanced Alternative Medicine Center
Serving All Your Heath Care Needs ... Naturally!
Dr. Richard A. Huntoon
Pooler Chiropractor
Newburgh Chiropractor

A winner of the 2015 Patients' Choice Awards in Chiropractic - Newburgh, NY
Verified by Opencare.com
Home | Chronic Health Concern | Specific Health Concern | My Child’s Health | Health and Wellness | New Patient Center | Other
Copyright © 2019 All Rights Reserved.